As you age, your digestive system undergoes physiological shifts that can turn your favorite meals into sources of discomfort, meaning you need to adapt your diet to maintain nutrient absorption and overall wellness. Modifying your intake of common trigger foods allows you to relieve bloating, acid reflux, and irregular bowel habits without sacrificing flavor or essential nutrients. Research indicates that reduced stomach acid production and changes in the gut microbiome directly impact how efficiently older adults process complex proteins and sugars. Understanding these biological changes empowers you to make informed dietary substitutions. You can protect your long-term health and digestive comfort by recognizing which ingredients prompt adverse reactions and replacing them with easily digestible alternatives.
The Science of Aging Digestion
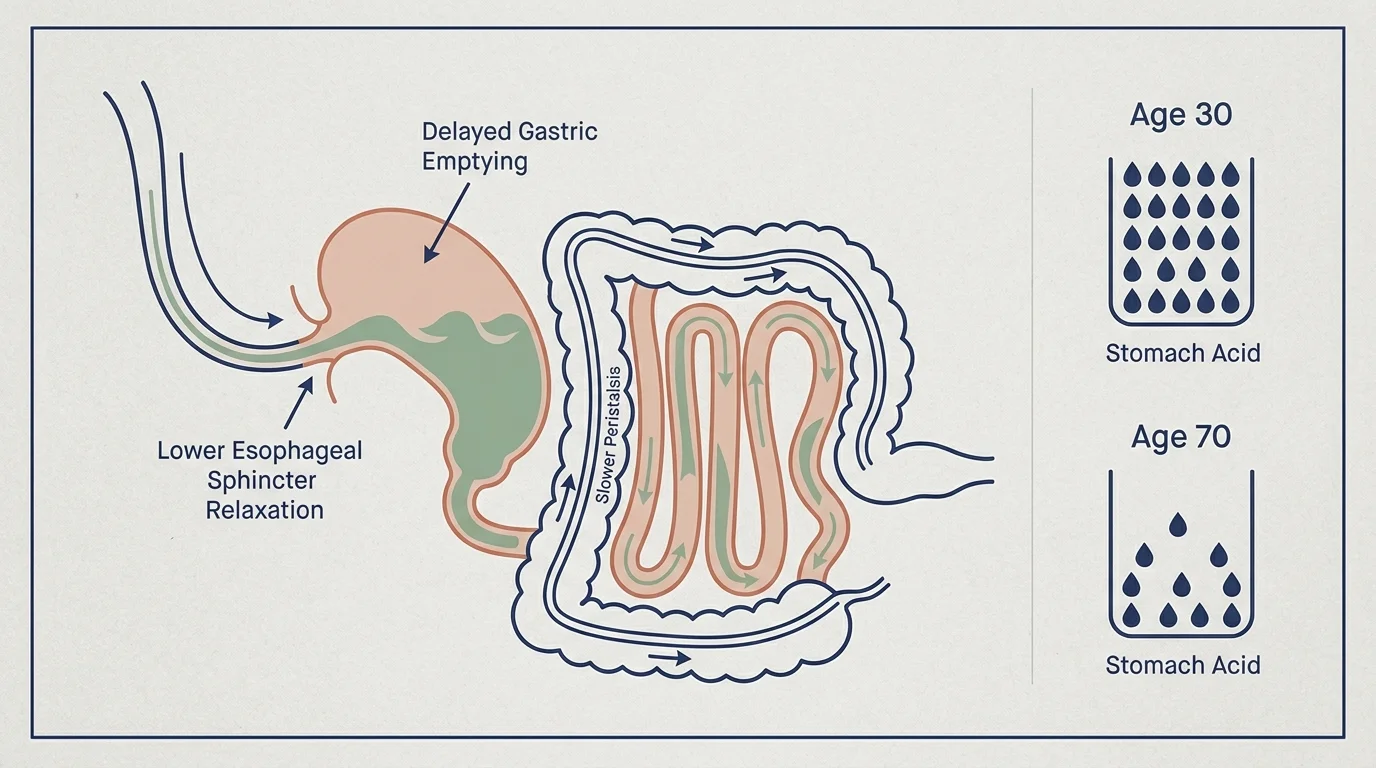
Your gastrointestinal tract operates differently at age seventy than it did at age thirty. Over the decades, the muscular contractions that move food through your digestive system—a process known as peristalsis—gradually slow down. This delayed gastric emptying means food remains in your stomach longer, increasing the likelihood of fullness, nausea, and acid reflux. Furthermore, your body naturally produces fewer digestive enzymes and less stomach acid as you get older. These chemical tools are essential for breaking down tough dietary fibers, complex carbohydrates, and dense proteins.
Simultaneously, the population of bacteria in your gut shifts. The diversity of your microbiome often decreases, reducing the presence of beneficial bacteria that help ferment dietary fiber and maintain an intact gut lining. A weakened lower esophageal sphincter often compounds these lower gastrointestinal changes; this small muscle normally keeps stomach acid from splashing upward, but its relaxation allows acidic contents to escape into the esophagus. Recognizing these underlying mechanisms, which align with digestive system changes documented by federal health researchers, helps you understand that new food intolerances represent a normal biological evolution rather than a personal failing.

8 Foods That Become Harder to Tolerate

1. Unfermented Dairy Products
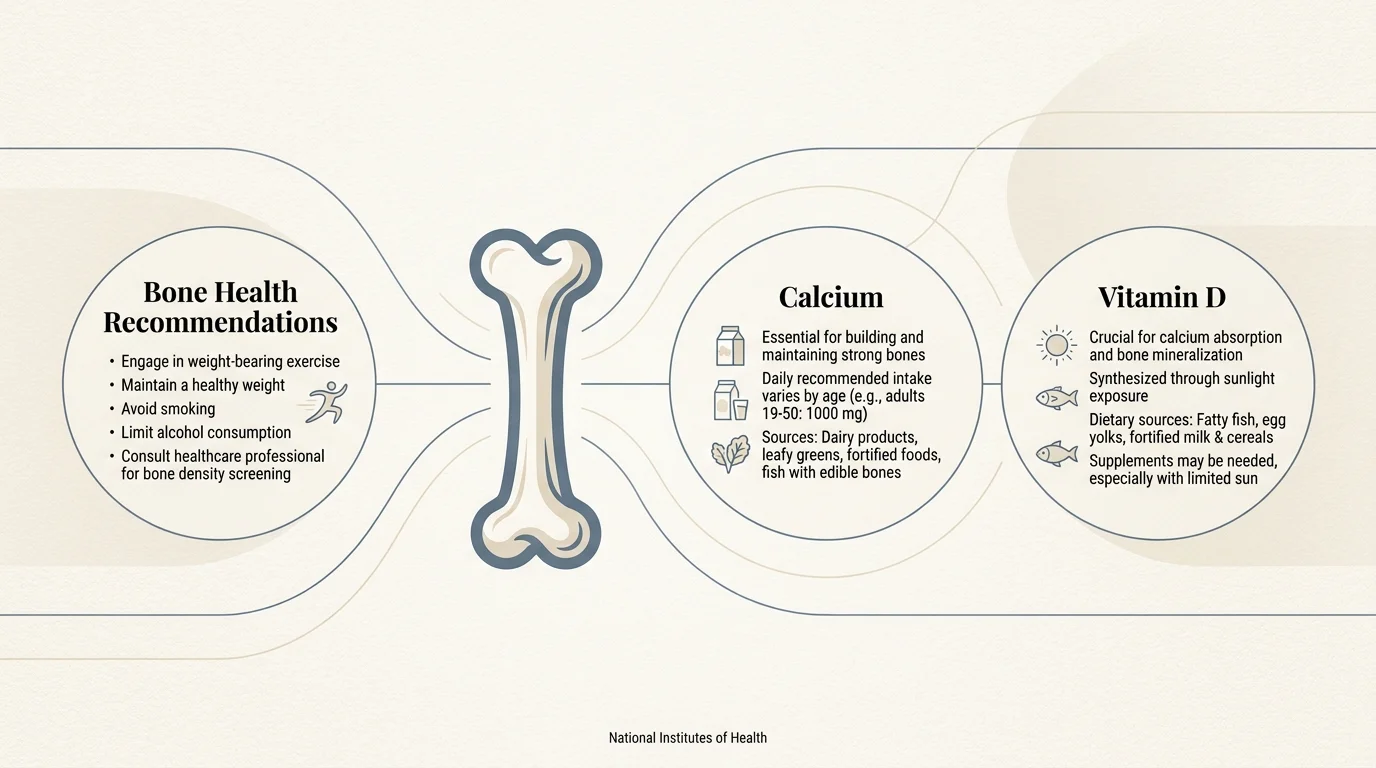
Many older adults suddenly find that a glass of cold milk or a bowl of ice cream results in severe cramping and bloating. This occurs because the production of lactase—the enzyme responsible for breaking down the milk sugar lactose—declines sharply with age. When undigested lactose reaches your colon, gut bacteria ferment it, creating excess gas and drawing water into the bowels. You do not have to abandon dairy entirely. You can transition to fermented options like plain kefir and Greek yogurt, which contain live cultures that pre-digest the lactose for you. Aged cheeses such as cheddar, Swiss, and Parmesan also contain negligible amounts of lactose and provide a safer way to secure bone health recommendations from the National Institutes of Health.

2. Deep-Fried and Greasy Meals
Fried chicken, French fries, and heavy cream sauces place a massive burden on an aging digestive tract. Dietary fats require significant bile and enzymatic action to digest, and they naturally slow the emptying of the stomach. For an older adult with sluggish peristalsis, a high-fat meal simply sits in the digestive tract, creating a sensation of profound sluggishness and triggering severe acid reflux. You can replicate the satisfying crunch of fried foods by investing in an air fryer or using high-heat oven roasting techniques. Brushing a light coat of olive oil on breaded chicken or potatoes yields a crispy texture while drastically reducing the digestive workload.

3. Highly Acidic Citrus and Tomato Products
Grapefruit, orange juice, and rich tomato sauces frequently trigger heartburn in older populations. The high acid content of these foods directly irritates the sensitive lining of the esophagus, especially when the lower esophageal sphincter no longer closes tightly. Tomato paste and concentrated sauces often cause more trouble than fresh, raw tomatoes. You can mitigate this acidity by modifying your recipes. Adding finely grated carrots or a small amount of baking soda to tomato sauce naturally neutralizes the acid without requiring refined sugar. For breakfast, you can swap acidic citrus juices for gentler alternatives like freshly blended melon or pear juice.

4. Raw Cruciferous Vegetables
Broccoli, cauliflower, cabbage, and Brussels sprouts belong to the cruciferous family, which boasts incredible cancer-fighting compounds but also contains raffinose. Raffinose is a complex carbohydrate that humans cannot digest on their own; we rely entirely on gut bacteria to ferment it. In an older digestive system with an altered microbiome, this fermentation produces painful trapped gas. You should prioritize cooking these vegetables thoroughly rather than eating them raw in salads. Steaming, roasting, or pureeing cruciferous vegetables into warm soups breaks down the tough cellulose fibers, allowing you to absorb the valuable nutrients without the agonizing afternoon bloat.

5. Spicy Peppers and Pungent Curries
Fiery dishes packed with hot chilies, cayenne pepper, and heavy curry powders frequently become intolerable as the mucosal lining of the stomach thins with age. Capsaicin, the active component that gives peppers their heat, acts as a chemical irritant that can provoke stomach spasms, cramping, and sudden diarrhea. You can still enjoy deeply flavorful meals without the gastrointestinal distress by pivoting your culinary strategy toward aromatic herbs. Fresh basil, cilantro, dill, thyme, and rosemary provide robust flavor profiles. Ground spices like turmeric, coriander, and mild cumin deliver warmth and complexity without irritating delicate digestive tissues.

6. Artificial Sweeteners and Sugar Alcohols
In an effort to manage blood sugar or reduce caloric intake, many older adults turn to sugar-free candies, gums, and diet beverages. Unfortunately, these products frequently contain sugar alcohols like sorbitol, xylitol, and erythritol. The human body absorbs these compounds poorly, and they draw massive amounts of water into the intestines, frequently causing urgent osmotic diarrhea. They also disrupt the delicate balance of the gut microbiome. You will achieve better digestive comfort by flavoring foods with small amounts of natural sweeteners, such as a teaspoon of real maple syrup or a dash of cinnamon and vanilla extract, which trick the palate into perceiving sweetness.
7. Ultra-Processed Cured Meats
Bacon, sausage, hot dogs, and deli meats combine multiple digestive antagonists into a single package. They are incredibly high in saturated fats, heavily preserved with nitrates, and packed with sodium. This combination aggressively slows digestion and promotes systemic inflammation. Breaking down these tough, processed animal proteins requires robust stomach acid, which older adults often lack. You can protect your gut by substituting these harsh meats with easily digestible lean proteins. Baked poultry, flaky white fish, tofu, and soft scrambled eggs provide necessary amino acids for muscle maintenance while demanding minimal effort from your digestive organs.

8. Raw Garlic and Onions
Raw alliums are potent sources of fructans, a type of fermentable carbohydrate that triggers severe bloating and abdominal pain in sensitive individuals. Because the aging gut frequently struggles with rapid fermentation, raw garlic in salad dressings or raw onions on sandwiches can ruin an otherwise comfortable day. You can capture the savory essence of these ingredients by using garlic-infused or onion-infused olive oils. The troublesome carbohydrates are water-soluble, meaning they do not seep into the oil, but the flavor compounds do. Alternatively, cooking onions and garlic slowly until they are deeply caramelized alters their chemical structure and significantly improves their digestibility.

Strategy Pillars for Digestive Health

Meal Planning Approaches
Rethinking your daily eating schedule often provides more relief than simply restricting ingredients. Your digestive tract functions best when it manages small, manageable workloads rather than massive influxes of food. You should transition from three heavy meals to four or five smaller, nutrient-dense meals spread evenly throughout the day. This approach prevents the stomach from becoming overstretched and ensures your limited supply of digestive enzymes can adequately process the food. Additionally, you should plan to consume your heaviest, most complex meals at midday rather than in the evening. Eating a large dinner right before bed forces your body to digest while lying flat, practically guaranteeing nocturnal acid reflux. Leave a window of at least three hours between your final bite of food and your bedtime.
Nutrient Focus
Balancing hydration and fiber intake becomes a daily necessity for an aging digestive system. While fiber is crucial for bowel regularity, older adults must increase their intake gradually to avoid sudden blockages or gas. Focus specifically on soluble fiber, which dissolves in water to form a soothing, gel-like substance in the gut. Excellent sources include oats, chia seeds, peeled apples, and soft-cooked root vegetables. You must pair this fiber with adequate fluid intake; without enough water, fiber acts like concrete in the intestines. Sipping warm liquids, such as ginger tea or bone broth, throughout the day stimulates digestive juices and fulfills the hydration guidelines published by the Academy of Nutrition and Dietetics without overwhelming your bladder all at once.

Habit Formation
The mechanical process of eating directly dictates your downstream comfort. Digestion begins in your mouth, where your teeth grind food and your saliva introduces amylase, an enzyme that targets carbohydrates. You must chew your food until it reaches a paste-like consistency, taking the physical burden off your stomach. Practice mindful eating by sitting upright at a table, entirely free from the distractions of televisions or smartphones. This presence of mind helps your nervous system shift into a relaxed state, which is required for optimal blood flow to your digestive organs. After completing a meal, you should resist the urge to recline on the couch. A gentle ten-minute walk around your neighborhood utilizes gravity to push food downward and accelerates the emptying of the stomach.

Expert and Lived Voices
Registered dietitians who specialize in geriatric nutrition frequently observe that patients endure years of unnecessary discomfort because they assume stomach pain is just a normal part of getting older. Clinical experts emphasize that dietary modification offers profound relief when applied consistently. Many older adults report that keeping a simple notebook in their kitchen transformed their relationship with food; by tracking what they ate alongside their physical symptoms, they identified specific triggers they previously overlooked. Community support groups for older adults continually echo the sentiment that sharing modified recipes—like swapping heavy cream for blended silken tofu in soups—helps maintain the joy of eating while respecting the body’s new physiological boundaries. This proactive mindset shifts the narrative from restriction to creative adaptation.
Safety and Personalization
While tweaking your diet safely manages age-related food intolerances, you must remain vigilant for symptoms that indicate more severe medical conditions. You should never ignore warning signs such as unintended weight loss, chronic nausea, difficulty swallowing, or black, tarry stools. These red flags require immediate evaluation by a physician to rule out ulcers, blockages, or malignancies. Furthermore, many medications commonly prescribed to older adults—including blood pressure drugs, joint pain relievers, and supplements—can aggressively irritate the stomach lining or induce constipation. You must review your complete medication list with a pharmacist or gastroenterologist to ensure your digestive distress stems from food rather than an adverse drug interaction. Always personalize these dietary strategies to accommodate your specific medical background, consulting a clinical professional before entirely removing broad food groups from your daily routine.
Frequently Asked Questions
Can food intolerances develop suddenly in your sixties or seventies?
Yes, developing a sudden intolerance to a lifelong favorite food is entirely normal in your later years. As your body ages, the cumulative drop in digestive enzymes, alterations in the gut microbiome, and changes in intestinal motility can reach a tipping point. A meal that caused zero issues at age fifty-five might trigger significant bloating at age sixty-five simply because your physiological capacity to process that specific combination of fats, proteins, or sugars has fundamentally changed. Medical professionals track these evolving sensitivities through peer-reviewed gastroenterology studies, confirming that gut composition is dynamic throughout your lifespan.
Is it necessary to completely eliminate a food if it causes mild discomfort?
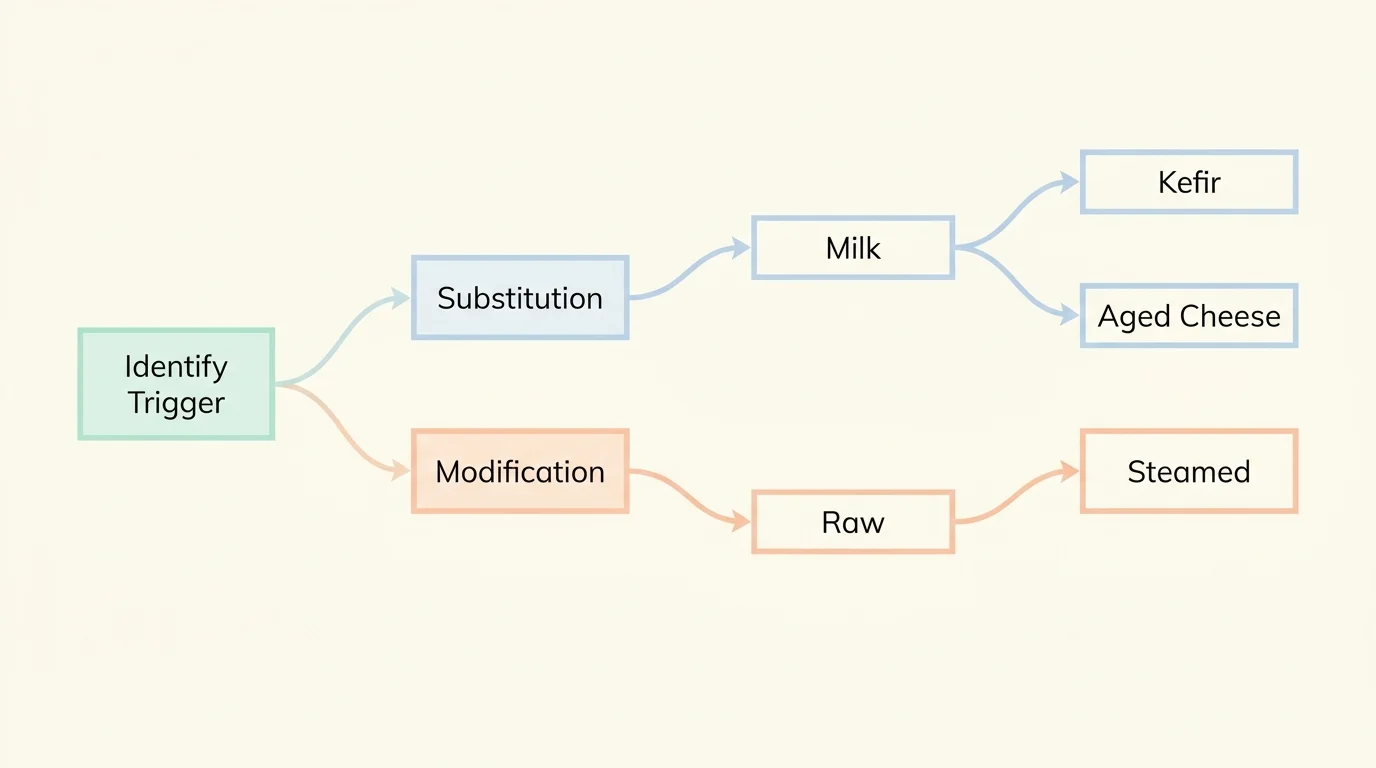
Complete elimination is rarely necessary unless you have a diagnosed allergy or celiac disease. In most cases of age-related food intolerance, your symptoms are entirely dependent on portion size and preparation methods. You might find that eating a large bowl of broccoli causes severe pain, but adding a half-cup of thoroughly steamed broccoli to a blended soup goes entirely unnoticed by your digestive tract. Experimenting with smaller quantities, different cooking techniques, and careful combinations allows you to maintain a diverse, nutrient-rich diet without suffering.
How can I get enough calcium if I can no longer tolerate dairy?
Protecting your bone density remains critical, and you can achieve your calcium goals without relying on fluid milk. Many non-dairy alternatives, such as almond, oat, and soy milks, are heavily fortified with calcium and vitamin D. Beyond fortified beverages, you can incorporate naturally calcium-rich foods like canned salmon with soft bones, sardines, dark leafy greens like kale and bok choy, and calcium-set tofu. If you still struggle to meet your daily requirements through food alone, you should discuss an appropriate calcium citrate supplement with your primary care provider, as calcium citrate digests more easily on a less acidic stomach than calcium carbonate.
Do digestive enzymes actually help older adults digest problem foods?
Over-the-counter digestive enzymes provide substantial relief for many older adults, provided you select the correct type for your specific trigger. Lactase supplements effectively mitigate the symptoms of lactose intolerance when taken just before consuming dairy. Alpha-galactosidase supplements help break down the complex carbohydrates found in beans and cruciferous vegetables, preventing the formation of excessive gas. However, broad-spectrum enzyme blends are not a universal cure for a poor diet. You should utilize them as a targeted tool alongside the clinical guidance from gastroenterologists and solid meal planning strategies.
Your Next Step for Better Digestion
Reclaiming your digestive comfort does not require overhauling your entire pantry overnight. Your most powerful tool is simple observation. Within the next twenty-four hours, commit to keeping a brief, honest record of everything you consume and how your stomach feels two hours later. Identifying just one major trigger—whether it is your morning orange juice or a heavy evening meal—gives you the exact target you need to make a meaningful substitution. You hold the power to restore your vitality; take that first step toward a calmer, more comfortable relationship with your food today.







